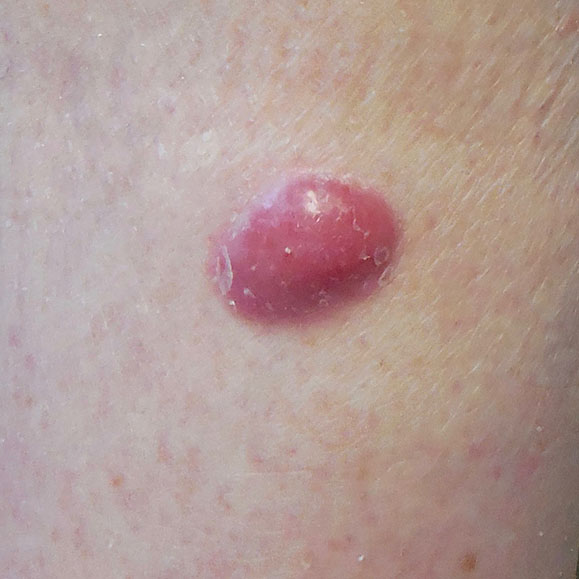
Merkel Cell Carcinoma
Home • Dermatology • Skin Cancer, Pre-Cancerous Lesions & Treatment • Merkel Cell CarcinomaCauses
Merkel cell carcinoma (MCC) is a rare but aggressive type of skin cancer that originates in the Merkel cells, found in the top layer of the skin near nerve endings. These cells play a role in touch sensation. MCC often develops on sun-exposed areas like the face, neck, and arms and is known for its rapid growth and potential to spread (metastasize) to other parts of the body, including lymph nodes and distant organs.
Although MCC is rare, its aggressive nature makes early detection and treatment critical.
What Causes Merkel Cell Carcinoma?
MCC occurs due to uncontrolled growth of Merkel cells, which is often triggered by a combination of factors:
- Merkel Cell Polyomavirus (MCPyV): This virus is detected in about 80% of MCC cases. While most people are exposed to MCPyV without consequences, genetic mutations caused by the virus in certain individuals can lead to MCC.
- UV Radiation: Prolonged exposure to ultraviolet (UV) radiation from sunlight or tanning beds can damage skin cells and contribute to MCC development.
- Weakened Immune System: People with compromised immune systems, such as organ transplant recipients or those with HIV/AIDS, are at higher risk.
- Chronic Sun Damage: Cumulative sun exposure over time increases the likelihood of MCC.
Risk
Although MCC is rare, the following populations face a higher risk:
- Older Adults: MCC is most commonly diagnosed in individuals over the age of 65.
- Fair-Skinned Individuals: Those with lighter skin tones are more susceptible to MCC, particularly in sun-exposed areas.
- Excessive Sun Exposure: Chronic sun exposure increases risk.
- Immunosuppressed Individuals: Conditions like HIV, certain cancers, or medications (e.g., immunosuppressants for organ transplants) heighten vulnerability.
- Males: Men are slightly more likely to develop MCC than women.
Symptoms
MCC typically appears as a painless, firm, red or purple nodule or bump on the skin. It often grows rapidly and may look like:
- A shiny, dome-shaped lump.
- A lesion with a bluish-red or skin-colored appearance.
- A sore that doesn’t heal.
These lesions most commonly occur on sun-exposed areas such as the face, neck, arms, and legs, but they can appear anywhere on the body. MCC lesions often lack specific symptoms, making them easy to overlook.
Diagnosis of Merkel Cell Carcinoma
Early detection is crucial due to MCC’s aggressive nature. Diagnosis typically involves:
- Skin Examination: Dermatologists visually inspect the lesion for characteristics of MCC.
- Biopsy: A sample of the lesion is removed and examined under a microscope to confirm MCC.
- Imaging Tests: CT scans, MRIs, or PET scans may be used to determine whether the cancer has spread to lymph nodes or other organs.
- Sentinel Lymph Node Biopsy: Often performed to check if cancer has reached nearby lymph nodes.
Treatment
Treatment for MCC depends on the stage of the disease and whether it has spread. A multidisciplinary approach combining surgery, radiation, and systemic therapies is often required.
- Surgical Treatments
- Wide Local Excision: Removal of the tumor along with a margin of healthy tissue to reduce the risk of recurrence.
- Sentinel Lymph Node Biopsy: Determines whether the cancer has spread to nearby lymph nodes. If cancer is found, a more extensive lymph node dissection may be required.
- Radiation Therapy
- Radiation is often used as an adjunct to surgery to target any remaining cancer cells or to treat inoperable tumors. It may also be used to manage MCC that has spread to lymph nodes or other areas.
- Systemic Therapies
For advanced or metastatic MCC, systemic treatments include:- Immunotherapy:
- Drugs like avelumab and pembrolizumab are FDA-approved for treating advanced MCC. These immune checkpoint inhibitors help the immune system recognize and attack cancer cells.
- Chemotherapy:
- Once the primary treatment for advanced MCC, chemotherapy is now less commonly used due to the availability of immunotherapy. It may still be an option in certain cases.
- Immunotherapy:
- Clinical Trials
- Innovative treatments, including novel immunotherapies and targeted therapies, are being studied in clinical trials, offering hope for patients with advanced disease.
Prevention
While not all cases of MCC can be prevented, the following steps can significantly reduce risk:
- Protect Skin from UV Radiation
- Use sunscreen with SPF 30 or higher daily.
- Wear sun-protective clothing, wide-brimmed hats, and sunglasses.
- Avoid tanning beds.
- Monitor Skin Changes
- Regularly examine your skin for new or changing growths, particularly if you have risk factors for MCC.
- Maintain Immune Health
- For individuals with weakened immune systems, regular skin check-ups are essential.
- Early Treatment of Lesions
- Act promptly on any suspicious lumps or lesions by consulting a dermatologist.
Prognosis and Importance of Early Detection
The prognosis for MCC depends on the stage at diagnosis:
- Localized MCC (no spread): The five-year survival rate is approximately 75%.
- Regional Spread (to lymph nodes): The survival rate decreases to about 50%.
- Distant Spread (metastasis): The five-year survival rate drops to roughly 25%.
Early detection and prompt treatment significantly improve outcomes. Regular follow-ups are essential, as MCC has a high recurrence rate.
Final Thoughts
Merkel cell carcinoma is a rare but aggressive skin cancer that requires swift diagnosis and treatment. Awareness of its symptoms and risk factors, coupled with regular dermatological screenings, is crucial for early detection. Advances in immunotherapy, particularly with drugs like avelumab and pembrolizumab, are revolutionizing the treatment of advanced MCC and offering new hope to patients.
By protecting your skin from UV damage, maintaining immune health, and seeking prompt care for suspicious lesions, you can reduce your risk and improve outcomes for Merkel cell carcinoma.
Prevention